STEVEN SOIFER, PhD, MSW
School of Social Work, University of Maryland, Baltimore, Maryland, USA
JOSEPH HIMLE, PhD, MSW
School of Social Work and Department of Psychiatry, University of Michigan, Ann Arbor, Michigan, USA
KATHLEEN WALSH, PhD, MSW
Millersville University, Millersville, Pennsylvania, USA
Paruresis is a social anxiety disorder characterized by a fear of being unable to urinate in the presence of others. This condition has not been covered in the social work literature, yet is a perfect example of a person-in-environment problem. This article explores the use of graduated exposure therapy during weekend-long workshops for the treatment of paruresis. One hundred and one participants participated in workshops and were administered pretreatment. posttreatment, and 1-year follow-up treatment scales. Repeated measures analysis of variance indicated significant improvement in shy bladder symptoms. Significant improvement in global severity of shy bladder was observed posttreatment and at the 1-year follow-up point. Findings suggest that graduated exposure therapy improves self-reported global severity of shy bladder symptoms and that these gains were maintained after a one-year follow-up.
KEYWORDS: shy bladder, bashful bladder, paruresis, social anxiety, public restrooms graduated exposure therapy
Received September 10, 2008; accepted November 19, 2009.
We express our immense appreciation to Cathy Costa, Research Assistant, for editing this article.
Address correspondence to Steven Soifer, PhD, MSY, Associate Professor, University of Maryland School of Social Work, 525 W. Redwood Street, Baltimore, MD 21201. E-mail: ssoifer@ssw.umaryland.edu
Page 1
| Paruresis (Shy Bladder Syndrome) |
PARURESIS: SHY BLADDER SYNDROME-—THE LATEST
SOCIAL PHOBIA?
Paruresis, more commonly known as shy or bashful bladder syndrome, is the fear of being unable to urinate (and often actually not being able to urinate in the presence of other people. While paruresis usually manifests itself in public restroom facilities, it is not uncommon for many people with paruresis to be unable to urinate in even their own homes when guests are present. People with paruresis may experience significant hardships in many areas of their lives such as interpersonal relationships, travel, and work, including problems with workplace drug testing (Soifer, Zgourides, Himle, & Pickering, 2001).
Approximately 17 million people in the United States, roughly 7% of the population, report that they have trouble using the restroom away from home (Kessler, Stein, & Berglund, 1998). Although all of these reported problems using the restroom cannot be attributed to paruresis, it is likely that many of these people suffer from this syndrome. The precise prevalence of paruresis in the general population is unknown. However, the prevalence is estimated to range from 2% to 50%, suggesting that It is a common problem and it appears to affect men and women equally and seems to be present in different areas of the world (Furmark, 2000; Gruber & Shupe, 1982; Hammerstein, Pietrosky, Merbach, & Braehler, 2005; Palmtag & Reidasch, 1980; Rees & Leach, 1975; Stein, Torgrud, & Walker, 2000; Williams Degenhardt, 1954).
Although the Diagnostic and Statistical Manual of Mental Disorders (2000) does not specifically mention paruresis, it does refer to the difficulty of using public restrooms as an example of a social phobia (social anxiety disorder). For some, the difficulty is very mild and presents itself as a “once in a blue moon” phenomenon, such as when in line for the restroom during the seventh-inning stretch at a baseball game. For others, though, this social anxiety disorder may become so severe that they essentially become homebound, limiting their outings to occasional short trips because the only “safe” bathrooms are in their houses (Soifer et al., 2001).
“While clearly a “private trouble,” paruresis is also a “public issue” that can be addressed through environmental interventions (Mills, 1959), and as such it offers special workers a perfect example of how a person-in-environment perspective (PIE) can be useful in understanding social anxiety and developing effective interventions. people with paruresis most commonly identify three triggers that are associated with difficulty urinating in public restrooms (Soifer et al., 2001). For the typical person with paruresis, these triggers must be managed for urination to occur (Soifer et al., 2001). The first of these triggers, is familiarity with other people present in the restroom, can trigger problems initiating urine, Conversely, some individuals with paruresis might find it easier to urinate around friends or relatives as opposed to strangers.
Page 2
| S. Soifer et al. |
Because of the personal nature of elimination, the degree of familiarity with and perceived acceptance of others in the room often determines whether the person with paruresis will successfully void (Soifer et al., 2001).
Second, proximity plays a role in the ability to initiate urine. Proximity for the person with paruresis is both physical, relating to the relative closeness of others in or near the restroom, and psychological, relating to the need for privacy, Many people with paruresis report significant distress and difficulty initiating urine when others are nearby (Soifer et al., 2001). This problem is especially challenging when suitable partitions between urinals and stall doors are not in place. When people with paruresis feel that their personal space has been invaded, they often report that they cannot initiate urine (Soifer et al, 2001). Better-designed restrooms, especially for men, would go a long way toward alleviating the problem of many who suffer from this disorder.
Third, temporary psychological states, especially anxiety, anger, and fear, can interfere with urination, Many people with paruresis are very concerned about the sounds and smells they make while urinating (Soifer et al, 2001). They also often worry that others will notice that they are or are not urinating and will criticize them for it, The influence of emotional states on the ability to urinate may in part explain why people with paruresis sometimes report difficulty urinating when they are overly excited or under pressure to hurry even when they are at home or using an isolated public restroom (Soifer et al,, 2001).
In addition to common triggers experienced by people with paruresis, certain behavioral patterns typify paruresis. For some people with paruresis, difficulty urinating in the presence of others appears to begin out of nowhere, but for most, the onset of the problem is associated with an unpleasant event(s). Common situations associated with the onset of paruresis include being harassed or teased by peers in a public restroom, being rushed to urinate by another person, and being unable to produce urine for a medical or drug test. Once individuals experience difficulty urinating, they often begin to worry about whether they will be able to urinate when confronted with needing to use a public restroom. The combined impact of the initial failure to urinate and the subsequent worry about failing again often produces increased sympathetic nervous system activity. This activity can create a level of anxiety that is incompatible with urinating (Zgourides, 1987). As each forcible attempt to control the process fails, greater increases in sympathetic nervous system activity further reduce the chances of successfully voiding. In many cases, this performance anxiety eventually generalizes to all or most public restrooms so that the only “safe” toilet the person can reliably use is at home (Zgourides, 1987).
Generally, people with paruresis try to adjust to the problem by urinating as often as possible when at home, restricting the intake of fluids, and: refusing extended social invitations, Most people with paruresis also engages in a series of protective behaviors
Page 3
| Paruresis (Shy Bladder Syndronie)|
such as locating vacant restrooms when away from home, thinking of water when trying to urinate, and running the tap to optimize the chances of urinating under adverse conditions. Most commonly, however, people with paruresis cope by avoiding public restrooms at all costs (Soifer et al., 2001).
LITERATURE REVIEW
Not surprisingly, there is no discussion of paruresis in the social work literature: Most of what has been written appears either in the urological or psychological literature. As this social anxiety disorder becomes more widely known, and given the large number of people it affects, the authors expect that more will be written about shy bladder syndrome in social work and the general health care literature. Moreover, because this issue is an excellent example of how a PIE perspective can illuminate a complex problem, it is ripe for social workers to address.
:: Urological literature reveals that early attempts to treat paruresis focused on surgical interventions. One favorite method of treatment was bladder neck ‘surgery (Winsbury-White, 1936). Surgery of the urethral sphincters was reported as late as the 1950s (Emmett, Hutchins, & McDonald, 1950). Freudian interpretations and psychoanalysis for the problem were reported in the psychological literature during the 1940s, 1950s, and early 1960s. In particular, case reports from Menninger (1941), Williams and Johnson (1956), Chapman (1959), and Wahl and Golden (1963) stand out (the fast of which mentioned men having this condition for the first time in the literature). While these case reports were often successful, psychoanalytic treatment often required several years before improvement was realized. It is also important to note that successful case reports do not indicate how many people with paruresis failed to improve with psychoanalysis.
“In their seminal article, Williams and Degenhardt (1954) coined the term paruresis, an important development given that as many as 36 other different terms for the disorder have been used over the years in the urologic literature (Soifer, Nicaise, Chancellor, & Gordon, 2009). Williams and Degenhardt also found through a survey an incidence rate of paruresis of 14% among students at one college, and they attributed the causes of the difficulties the students experienced with urination to anxiety in social situations.
Starting in the mid-1960s and through the 1970s, clinicians began to use more behavioral approaches in treating paruresis beginning with counter-conditioning (Cooper, 1965; Wilson, 1973). Others followed suit by utilizing whole range of behavioral therapy techniques, such as in vivo desensitization (Anderson, 1977; Elliott, 1967), flooding (Lamontagne & Marks, 1973), conditioned relaxation (Ray & Morphy, 1975), systematic desensitization in combination with relaxation training (Glasgow,
Page 4
| S. Soifer et al. |
1975), paradoxical intention (Ascher, 1979), and multi-modal behavioral therapy (Montague & Jones, 1979.
These studies laid the groundwork for more sophisticated behavioral treatments implemented in the 1980s and 1990s, including the continued use of paradoxical intention (Jacob & Moore, 1984) and multi-modal behavioral therapies (Markway, Carmin, Pollard, & Flynn, 1992; Nicolau, Toro, & Prado, 1991), in vivo desensitization in combination with furosemide (a diuretic) to increase urgency (Thyer & Curtis, 1984), in vivo therapy with a portable radio headset to block out sounds (Zgourides, Warren, & Englert, 1990), in vivo desensitization in combination with relaxation training (McCracken & Larkin, 1991), cognitive restructuring in combination with graduated in vivo exposure (Jaspers, 1998), and respondent conditioning (Watson & Freeland, 2000). It should be noted that there are also two case reports of the successful treatment of paruresis with hypnosis (Mozdzierz,1985; Seif, 1982).
As clinicians began to use behavioral approaches to treating paruresis in the 1970s, medication began to be prescribed for paruresis, either as a stand-alone or an adjunct to therapy. Montague and Jones (1979); Stams, Martin, and Tan (1982); Kawabe and Niijima (1987); Hatterer et al. (1990); Zgourides and Warren (1990); and Bohn and Sternbach (1997) used or reported on a variety of drugs, including alpha-blockers, beta-blockers, benzodiazepines, and selective serotonin reuptake inhibitors (SSRIs) with mixed results. To date, there is no medication known that will “cure” paruresis.
Beginning in the 2000s, more sophisticated analyses and studies of paruresis have appeared in the literature. A survey by Vythilingum, Stein, and Soifer (2002) indicated that only about 50% of those with paruresis have co-morbid symptoms. Hammerstein and Soifer (2006) collected data that indicates paruresis may be more than just a social phobia and may actually be more a functional urination disorder, It is possible that there may be different forms of paruresis, some that may be forms of social phobia and some that may be more physical. Most recently, Boschen (2008) has presented a cognitive and behavioral model for understanding paruresis. This model incorporates an intervention strategy based on empirical evidence from treatment of other anxiety disorders.
CURRENT TREATMENT APPROACH
The formation of the International Paruresis Association (IPA) in 1996 took the treatment of paruresis to a new level. Building on the work of Joseph Himle, Ph.D., at the University of Michigan Anxiety Disorders Program, where the individual treatment of people with paruresis from a behavioral perspective had been occurring since the early 1990s, the co-founders of Outcome studies for CBT IPA, Steven Soifer, Ph.D.,
Page 5
| Paruresis (Shy Bladder Syndrome) |
and Carl Robbins, M.S., created a weekend workshop to treat people with paruresis. Soifer is more of a behaviorist, and Robbins is more of a cognitive therapist; consequently, they decided to use a cognitive-behavioral therapy (CBT) approach to the workshops that included graduated exposure.
CBT approaches that use graduated exposure have become the treatment of choice for phobias since the late 1970s (Dobson, 2001). CBT assumes that patterns of cognition shape the emotional and behavioral consequences of that cognition”(Dobson, 2001, p. ix). Given the variety of both cognition and behavioral techniques involved in this treatment approach in this system and the nature of paruresis, CBT allows for some flexibility in approach for dealing with different symptoms among clients but most importantly provides a consistent treatment framework for the anxiety disorder.
Outcome studies for CBT in the treatment of phobias are quite good. In particular, the recent meta-study by Butler, Chapman, Forman, and Beck (2006) shows that CBT works well not only for anxiety disorders but also for many other problems and that its general success rate is about 80% or better. A form of CBT graduated exposure, has demonstrated efficacy in the treatment of phobic clients. Based on the principles of operant conditioning, graduated exposure techniques instruct phobic clients to gradually stay longer in phobic situations (Emmelkamp, Bouman, & Scholing, 1992). There is no other treatment approach with as extensive an evidence base for social anxiety disorder and social phobia, and that is why CBT, including graduated exposure, has been used since the founding of IPA in its effort to treat paruresis.
IPA began to offer weekend workshops for the treatment of paruresis in 1997. With the advent of the Internet, people with this “secret” phobia could now anonymously access the World Wide Web and with increasing ease find an organization and program for dealing with paruresis. From the very beginning, IPA has never needed to advertise its workshops other than on its website; rarely are workshops canceled for lack of enrollment. Often, those who enroll have seen several health and mental health professionals to no avail. They report that finding people knowledgeable about paruresis is very difficult, especially professionals who could actually help them. The professionals the workshop attendees saw often learned about this anxiety disorder for the first time from their patients or clients.
There are very few trained CBT clinicians treating paruresis, and this also fuels the need for weekend workshops. By offering these weekend workshops in the largest U.S. cities (and eventually in cities outside the United States), IPA helped fulfill a need. While a number of the workshop participants were local to the hosting cities, often people would travel, sometimes even great distances, to attend these workshops. Ironically, sometimes people would choose to travel to workshops far away from home
Page 6
| S. Soffer et al. |
(eg, a man from England who attended a workshop in Texas) to make sure they would not run into someone they knew.
After each workshop, the workshop facilitator encourages the formation of a support group in the area in which the workshop was held. Often, support groups formed and thrived, but in some cases, the support groups never got off the ground or faltered. Nonetheless, support groups helped to provide a supportive environment in which many workshop attendees and others from the general public could come to practice techniques and recover from this sometimes debilitating disorder.
Finally, sufferers of paruresis who attended the workshops were encouraged to tell others, especially significant others, family members, relatives, and friends about their problem in order to lessen the feelings of isolation many people with paruresis experience and to help create a more supportive environment following the workshop. Feelings of shame and embarrassment often interfere with sufferers’ ability to tell others, but the act of doing so is frequently an important part of recovery.
METHOD
Overview
From 1997 through 2003, the investigators offered weekend workshops throughout the United States to people with paruresis in several major cities, These workshops included group-sharing techniques (Friday night) and the latest in cognitive-behavioral therapy methods (Saturday and Sunday) and were meant to help people begin to recover from paruresis. Participants typically paid $300 to attend the workshop; in a few cases, the payment was less or more because participants could choose to pay either the $300 flat fee or 1% of their gross income. A description of the participants and how they were recruited, measures, and a description of the workshops follow.
Participants
The participants were 101 people (89 male and 12 female) seeking treatment for paruresis who responded to website postings or were referred by professionals to attend a 3-day paruresis workshop held at a local hotel in one of five major U.S. cities. The size of the groups (7 = 5) ranged from 5 to 35 participants with a mean of 20.2 participants. The two larger groups (35 and 28 participants) were led by two, rather than one, clinicians, The mean age of the participants was 39.4 years (SD = 10.6). Participants reported experiencing symptoms for an average of 25.9 years (SD = 10.6) prior to attending the workshop.
Page 7
| Paruresis (Shy Bladder Syndrome) |
Measures
Primary outcome measures included the Bashful Bladder Scale (available “from the senior author), a 12-item inventory that measures the ability to urinate in several common phobic situations. The Bashful Bladder Scale yields a “total raw score from 0-48 with scores of 0-10 considered to be sub-clinical, and scores of 11-20, 21-30, and 31-48 indicating mild, moderate, and severe bashful bladder, respectively. This scale was administered at the very beginning of the workshop, at the very end of the workshop, and sent by e-mail to participants 1 year after the workshop. At the 1-year follow-up point,
The scale was completed by more than 95% of the participants, that is, 96 of 101 participants responded, This high respondent rate was achieved through several reminder e-mails and phone calls to participants.
The second primary outcome measure was a patient-rated global paruresis severity scale, which ranges from 0 (x20 symptoms) to 10 (extreme paruresis). This scale was also administered at the beginning of the workshop, at the end of the workshop, and to participants 1 year after the workshop. Workshop satisfaction was rated on a 0 (none) to 4 (enormously) scale of general satisfaction with the workshop. No formal reliability or validity claim is available for these measures.
Workshop Description
Workshops were led by one to two mental health professionals who were trained in the cognitive-behavioral treatment of paruresis. These professionals were either licensed social workers or psychologists. Workshops were held on weekends from Friday through Sunday in hotels with a conference room for group meetings and several different restroom opportunities for practice. The following is a typical weekend workshop schedule:
Friday, 7:00 p.m. to 10:00 p.m.
Introductions
Sharing our stories
Workshop Overview
Constructing behavioral hierarchies
Saturday, 9:00 am. to 5:00 p.m
Historical overview of paruresis
Behavioral (graduated exposure) approach to treating paruresis
Setting up the Buddy System
Graduated exposure exercises: Rounds 1-4
Debriefing
Questions and answers
The International Paruresis Association
Page 8
| S. Soifer et al. |
Sunday, 9:00 a.m. to 3:00 p.m.
Check-ins
Questions and answers
Graduated exposure exercises: Rounds 5-7
Where do you go from here?
Wrap-up and evaluation
On the first day (Friday from 7:00 p.m. to 10:00 p.m.), workshop participants share their personal stories about paruresis and how it has impacted their lives. Participants develop and discuss their personal behavioral exposure hierarchies, which include their continuum of fears ranging from the worst possible scenario (e.g., for men, this may be standing in front of a large trough-like urinal where people are shoulder to shoulder with one another) to situations in which they are the most comfortable (e.g., alone in one’s own home). During this session, participants start “buddying up” to develop practice dyads and triads so that they can begin the graduated exposure process. Typically, participants select partners with similar hierarchies.
On the second day of the workshop (Saturday from 9:00 a.m. to 5:00 p.m.), the workshop facilitator opens with a historical overview of paruresis, including information about its medical and psychological origins as well as various treatment modalities, The facilitator provides a detailed description of the graduated exposure process and asks the participants to begin working on the least anxiety-producing scenarios in their behavioral hierarchies.
Exposure partners then begin their practice sessions. Throughout the course of the workshop, participants drink fluids so that they have enough urine available for repetitive exposure practice. During the morning portion of the workshop, there are 1-2 practice sessions of about 45 minutes each in duration, wherein participants and their respective “buddies” practice the graduated exposure technique and attempt to void in various settings, moving up their own behavioral hierarchies. Participants typically start with the least difficult level of their hierarchies and work upward under their own control and at their own pace. The afternoon hours are reserved for additional practice opportunities and exposure to a restroom in the community outside the hotel if participants have progressed sufficiently.
On the final day of the workshop (Sunday from 9:00 a.m. to 3:00 p.m.), participants convene and participate in another 2-4 graduated exposure sessions. Participants are then given the opportunity to reflect on their experiences, identify successes and challenges, and develop strategies for how they will continue their progress after completion of the workshop. Participants are asked to identify practice buddies in their home area and are strongly encouraged 10 participate in support groups, online chats sponsored by IPA, and other methods of support. A more detailed description of workshop activities can be found in Chapter 1 of Soifer et al. (2001).
Page 9
| Paruresis (Shy Bladder Syndrome) |
Repeated measures analysis of variance indicated significant improvement in Bashful Bladder Scale Total Scores from pretreatment to posttreatment to 1-year follow-up (df = 2, f = 45.62, p < 000; see Figure 1). Participants improved from the middle of the “moderate” to the low end of the “moderate” range of the Bashful Bladder Scale from the beginning of the workshop to 1-year follow-up.
Significant improvement in the global severity of bashful bladder was also observed from pretreatment to 1-year follow-up df = 97, 1 = 6.856, p< 0001; see Figure 2).
Finally, high levels of participant satisfaction with the weekend workshop were observed (mean = 3.18 [SD = .67]; see Figure 3).
DISCUSSION
The central finding of this study is that graduated exposure therapy improves self-reported global severity of paruresis. Furthermore, the gains reported by participants were maintained at the 1-year follow-up point. Clinical impressions suggest that continued practice with graduated exposure techniques after the initial treatment intervention during the follow-up period was critical to maintaining and extending positive outcomes that were observed posttreatment. However, the authors do not have data to support the benefits of further exposure. Although the improvement in bashful bladder symptoms was modest, this study suggests that brief graduated exposure therapy provided over a weekend can decrease the severity of paruresis.
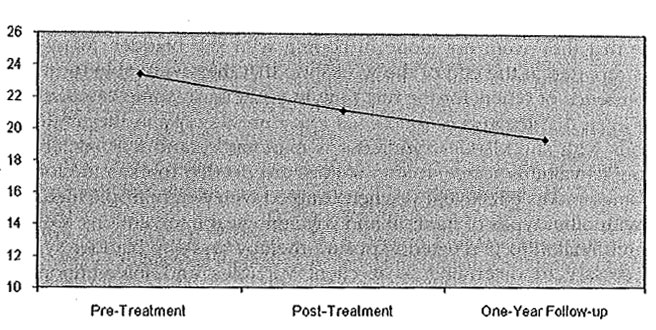
FIGURE 1 Bashful Bladder Scale Total Score changes from pretreatment to posttreatment to 1-year follow-up.
Page 10
| Soifer ef al. |
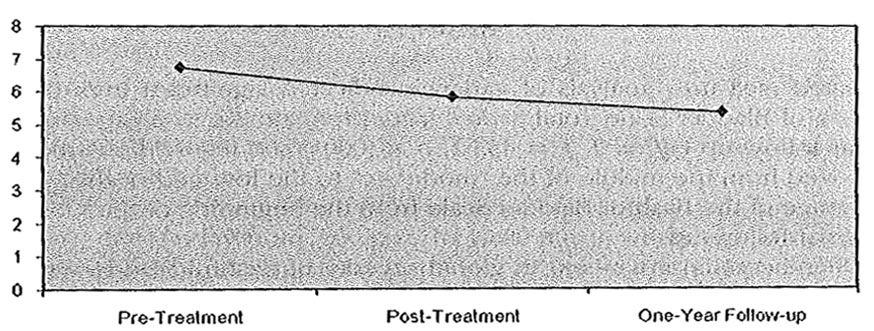
FIGURE 2 Global severity of paruresis changes from pretreatment 10 posttreatment to 1-year follow-up.
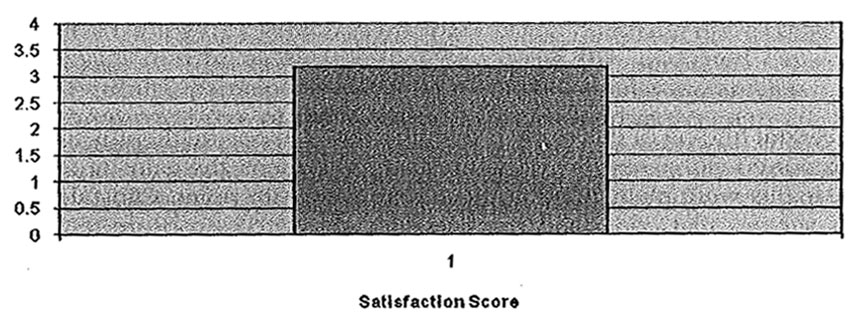
FIGURE 3 Average satisfaction with workshop immediately posttreatment.
Participants also reposted high levels of satisfaction with the workshops. Anecdotal reports indicate that the participants felt reduced feelings of shame enjoyed the support of their peers and benefited from the sense that they were not alone in coping with shy bladder. Many participants reported at the end of the workshop that they were able to urinate in the presence of others for the first time in years or, in some cases, ever.
Given that the use of graduated exposure therapy in the treatment of persons with shy bladder syndrome is exploratory and that research supporting its value is scarce, further studies are needed to examine long-term outcomes and its effectiveness when coupled with psychotropic medications and with other types of medical and psychological interventions. Continued research related to graduated exposure therapy and shy bladder syndrome is necessary to determine what client variables and intervention/group facilitators’ characteristics are associated with improvement In syndrome. Additionally, clinical impressions suggest extending the length of the workshop and/ or encouraging participants to join support or practice groups after the initial treatment may also improve outcomes.
Page 11
| Paruresis (Shy Bladder Syndronie) |
The results of this study need to be viewed with some caution. First, an important limitation of this study is the absence of a control group. Additional research is in order to determine whether exposure therapy intervention was responsible for the observed improvement or whether the gains were due to non-specific effects associated with the therapeutic milieu is needed. Second, the Bashful Bladder Scale may not be sensitive enough to detect the level of improvement observed after the completion of the workshop. Finally, the self-report method utilized by the Bashful Bladder Scale indicates only what participants say about their improvements and may not accurately reflect their true feelings and/or actual improvement in the ability to urinate.
The implications of this study for social work are important. There is a large population of people suffering from a newly identified social anxiety disorder, paruresis, who need treatment. As there is relatively little information available about shy bladder and few professionals trained to treat it, it would behoove social workers to learn about this phobia and become
skilled in helping people overcome it. There are a handful of mental health professionals worldwide treating this widely experienced social anxiety disorder. There is a great need not only for workshops to help these individuals but also for licensed clinicians, preferably social workers, to help people with paruresis on a one-to-one basis. This client population deserves nothing less, and social workers have the compassion and knowledge base to make a real difference in their lives.
REFERENCES
American Psychiatric Association. (2000). Diagnostic and Statistical Manual of Mental Disorders (4th ed., text revision). Washington, DC: Author.
Anderson, LT. (1977). Desensitization in vivo for men unable to urinate in a public facility, Journal of Behavior Therapy and Experimental Psychiatry, 8(1), 105-106.
Ascher, LM. (1979). Paradoxical intention in the treatment of urinary retention, Behavior Research and Therapy, 17(3), 267-270.
Bohn, I, & Sternbach, H. (1997). Current knowledge and research directions in the treatment of paruresis, Depression, and Anxiety, 5(1), 41-42.
Boschen, MJ. (2008). Paruresis (psychogenic inhibition of micturition): Cognitive behavioral formulation and treatment, Depression and Anxiety, 25(11), 903-912.
Butler, A.C., Chapman, J.E., Forman, E.M., & Beck, A.T. (2006). The empirical status of cognitive-behavioral therapy: A review of meta-analyses. Clinical Psychology Review, 26(1), 17-31.
Chapman, AH. (1959). Psychogenic urinary retention in women: Report of a case.Psychosomatic Medicine, 21(2), 119-122.
Cooper, AJ. (1965). Conditioning therapy in hysterical retention of urine. British Journal of Psychiatry, 111(476), 575-577.
Page 12
| S.Soifer et al. |
Dobson, K.S. (Ed). (2001). Handbook of Cognitive-Behavioral Therapies (2nd ed.). New York: Guilford Press.
Elliott, R. (1967). A case of inhibition of micturition: Unsystematic desensitization, The Psychological Record, 17(4), 525-530.
Emmelkamp, PM.G., Bouman, T.K., & Scholing, A. (1992), Anxiety Disorders: A Practitioner’s Guide. New York: John Wiley & Sons.
Emmett, JL, Hutchins, S.P.R., & McDonald, J.R. (1950). The treatment of urinary retention in women by transurethral resection. Journal of Urology, 63(6), 1031-1042.
Furmark, T. (2000). Social Phobia: From Epidemiology to Brain Function. Uppsala, Sweden: Acta Universitatis Upsalienss.
Glasgow, RE. (1975). In vivo exposure in the treatment of urinary retention, Behavior Therapy, 6(5), 701-702.
Gruber, D.L,, & Shupe, D.R. (1982). Personality correlates of urinary hesitancy paruresis and body shyness in male college students. Journal of College Student Personnel, 23(4), 308-313,
Hammelstein, P., Pietrosky, R., Merbach, M., & Braehler, E. (2005). Psychogenic urinary retention (“paruresis”): Diagnosis and epidemiology in a representative male sample. Psychotherapy and Psychosomatics, 74(5), 308-314.
Hammelstein, P., & Soifer, 5. (2006). Is “shy bladder syndrome” (paruresis) correctly classified as a social phobia? Journal of Anxiety Disorders, 20(3), 296-311.
Hatterer, J.A., Gorman, J.M., Fyer, AJ., Campeas, R.B,, Schneier, FR., Hollander, E., Liebowitz, MR. (1990). Pharmacotherapy for four men with paruresis. American Journal of Psychiatry, 147(1), 109-111.
Jacob, R.G., & Moore, DJ. (1984). Paradoxical interventions in behavioral medicine, Journal of Behavior Therapy and Experimental Psychiatry, 15(3), 205-213,
Jaspers, J.P. (1998). Cognilive-behavioral therapy for paruresis: A case report. Psychological Reports, 83(1), 187-196.
Kawabe, K., & Niijima, T. (1987). Use of an alpha 1-blocker, YM-12617, in micturition difficulty. Urologia Internationalis, 42(4), 280-284,
Kessler, R.C., Stein, M.B., & Berglund, P. (1998). Social phobia subtypes in the national comorbidity survey. American Journal of Psychiatry, 155(5), 613-619.
Lamontagne, Y., & Marks, 1.M. (1973). Psychogenic urinary retention: Treatment by prolonged exposure. Behavior Therapy, 4(4), 581-585.
Markway, B.G., Carmin, CN, Pollard, CA. & Flynn, T. (1992). Dying of Embarrassment: Help for Social Anxiety and Phobia. Oakland, CA: New
Harbinger,
McCracken, LM., & Larkin, K.T. (1991). Treatment of paruresis with in vivo desensitization: A case report. Journal of Behavior Therapy and Experimental Psychiatry, 22(1), 57-62.
Menninger, K.A. (1941). Some observations on the psychological factors in urination and genito-urinary afflictions. Psychoanalytic Review, 28, 117-129,
Mills, CAV. (1959). The Sociological Imagination, New York: Oxford University Press.
Montague, D.K., & Jones, L.R. (1979). Psychogenic urinary retention. Urology, 13(1), 30-35.
Mozdzierz, G.J. (1985). The use of hypnosis and paradox in the treatment of a case of chronic urinary retention/”bashful bladder.” American Journal of Clinical Hypnosis, 28(1), 43-47.
Page 13
| Paruresis (Shy Bladder Syndrome) |
Nicolau, R., Toro, J., & Prado, C.P. (1991). Behavioral treatment of a case of psychogenic urinary retention. Journal of Behavior Therapy and Experimental Psychiatry, 22(1), 63-68.
Palmtag, H., & Reidasch, G. (1980). Psychogenic voiding patterns. Urologia Internationals, 35(5), 321-327.
Ray, I, & Morphy, J. (1975). Metronome-conditioned relaxation and urinary retention, Canadian Psychiatric Association Journal, 2002), 139- 141.
Rees, B., & Leach, D. (1975). The social inhibition of micturition (paruresis): Sex similarities and differences. journal of the American College Health Association, 23(3), 203-205.
Seif, B. (1982). Hypnosis in a man with fear of voiding in public facilities. American Journal of Clinical Hypnosis, 24(4), 288-289,
Soifer, S., Nicaise, G., Chancellor, M., & Gordan, D. (2009). Paruresis or shy bladder syndrome: An unknown urologic malady? Urologic Nursing, 292), 87-93.
Soifer, 8., Zgowrides, G.D., Himle, J., & Pickering, N.L. (2001). Shy Bladder Syndrome: Your Step-by-Step Guide to Overcoming Paruresis. Oakland, CA; New Harbinger.
Stams, U.K., Martin, C.H., & Tan, T.G. (1982). Psychogenic urinary retention in an eight-year-old boy. Urology, 20(1), 83-85.
Stein, M.B., Torgrud, LJ., & Walker, J.R. (2000). Social phobia symptoms, sub-types, and severity: Findings from a2 community survey. Archives of General Psychiatry, 57(11), 1046-1052.
Thyer, B.A., & Curtis, G.C. (1984). Furosemide as an adjunct to exposure therapy of psychogenic urinary retention. Perceptual and Motor Skills, 5901), 114.
Vythilingum, B., Stein, DJ., & Soifer, S. (2002). Is “shy bladder syndrome” a subtype of social anxiety disorder? A survey of people with paruresis. Depression and Anxiety, 16(2), 84-87.
Wahi, C.W., & Golden, J.5. (1963). Psychogenic urinary retention: Report of 6 cases, Psychosomatic Medicine, 25(6), 543-555.
Watson, T.5., & Freeland, J.T. (2000). ‘Treating paruresis using respondent conditioning. Journal of Behavior Therapy and Experimental Psychiatry, 31(2), 155-162.
Williams, G.W., & Degenhardt, ET. (1954). Paruresis: A survey of a disorder of micturition. Journal of General Psychology, 51, 19-29,
Williams, G.E., & Johnson, A.M. (1956). Recurrent urinary retention due to emotional factors: Report of a case. Psychosomatic Medicine, 18(1), 77-80.
Wilson, G.T. (1973). Innovations in the modification of phobic behaviors in two clinical cases, Behavior Therapy, 4(3), 426-430,
Winsbury-White, H.P. (1936). Two cases of retention of urine in women. The Lancet, 227(5879), 1008-1009.
Zgourides, G.D. (1987). Paruresis: Overview and implications for treatment. Psychological Reports, 60(3), 1171-1176.
Zgourides, G.D., & Warren, R. (1990), Propranolol treatment of paruresis (psychogenic urinary retention): A brief case report. Perceptual and Motor Skills, 71(3), 885-886,
Zgourides, G.D., Warren, R., & Englert, M. (1990). Use of a portable radio headset as an adjunct to exposure therapy in treating paruresis. Phobia Practice and Research Journal, 3(1), 43-44.










inventore temporibus veniam temporibus non quis ea sed est molestiae velit accusantium. facere autem inventore saepe quas.